To lessen the risk of Suboxone addiction, the medication’s therapeutic benefits must be assured by appropriate usage under medical supervision. Misusing the drug can lead to dependency, and abrupt cessation can lead to withdrawal symptoms.
Detoxification and Suboxone addiction treatment involves gradually reducing the dosage. Get the facts about Suboxone rehab at We Level Up Texas Treatment Center. Make this your opportunity to reclaim your life. Call us for consultation. Every call is free and confidential.
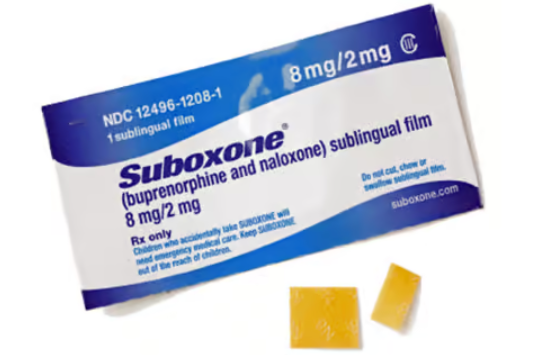
What is Suboxone?
Suboxone is a prescription that has the combination of naloxone and buprenorphine to treat opiate dependence.
The prescription Suboxone, which binds to the same brain receptors as opioids, lessens cravings and the symptoms of withdrawal from opioids. Unfortunately, though it is designed for addiction treatment, some users also misuse it.
Abusers of illegally obtained Suboxone, also known as “subs,” may crush and inject the drug, which is available as pills or dissolvable strips. When heroin isn’t available, many individuals who abuse Suboxone use it to escape withdrawal rather than receiving treatment. Some individuals who receive legal prescriptions might also develop addictions through unethical tactics like doctor shopping. Furthermore, people who lack an opiate tolerance may use Suboxone to get high, putting them at risk for dependence and a possible jump to heroin or more dangerous opioids.
Suboxone Addiction Signs
Psychological and behavioral signs of suboxone addiction:
- Craving for Suboxone.
- Compulsive thoughts about using the medication.
- Preoccupation with obtaining and using Suboxone.
- Loss of interest in once enjoyable activities.
- Continued use despite negative consequences.
- Difficulty in controlling or stopping Suboxone use.
- Increased tolerance, requiring higher doses for the same effect.
- Denial or minimizing the extent of Suboxone use.
- Irritability or mood swings when not using Suboxone.
Physical signs of suboxone addiction:
- Nausea or vomiting.
- Slurred speech.
- Drowsiness or sedation.
- Poor coordination.
- Constricted pupils.
- Respiratory depression (slow or shallow breathing).
- Constipation.
- Sweating or chills.
- Weight loss.
- Changes in sleep patterns.
Skip To:
Learn More:
How Does Suboxone Work?
Suboxone, which has buprenorphine and naloxone, helps to stop opioid harm and reduces withdrawal risk.
Buprenorphine helps with opioid recovery by easing withdrawal, and it’s hard to abuse it because it has a limit on its effects. Suboxone works like methadone but with less risk. Buprenorphine is a potent analgesic acting on the central nervous system (CNS).
The off-label use of buprenorphine is limited to injection and includes perineural anesthesia, as well as withdrawal management in hospitalized patients dependent on heroin. Naloxone, on the other hand, reverses opioid overdose effects by quickly blocking the opioids’ impact on the body’s respiratory and CNS. This powerful combination helps many patients to overcome opioid abuse.

How Long Does It Take to Get Addicted to Suboxone?
Buprenorphine has mild effects, making it less addictive than other opioids. However, misuse of Suboxone, which contains buprenorphine, has become a problem. For instance, some use it to extend heroin use.
If you are abusing Suboxone, you can become addicted to it in a matter of a few weeks. Nevertheless, some people may develop dependence much quicker, while others can take a bit longer.
The most common risk factors of Suboxone addiction are:
- Compulsive drug-seeking behavior.
- Increasing tolerance.
- Using Suboxone in ways other than prescribed.
- Inability to cut down or control use.
- Using Suboxone to cope with emotional or psychological issues.
- Craving for Suboxone.
- Suboxone withdrawal symptoms when discontinued.
Suboxone Side Effects Chart
| Category | Side Effects |
|---|---|
| Physical | Nausea, vomiting, constipation, drowsiness, headache, sweating, dizziness |
| Psychological | Anxiety, depression, insomnia, irritability, mood swings |
| Behavioral | Compulsive drug-seeking, neglecting responsibilities, increased tolerance |
| Other | Allergic reactions, difficulty breathing, liver problems, withdrawal symptoms with abrupt discontinuation |
Tips on How to Take Suboxone Safely
Suboxone is available in two forms: an oral film and a tablet. Both the film and the tablet are sublingual drugs. This means a patient should place the tablet under their tongue or between the tongue and cheeks, where it will dissolve.
People can drink water to moisten their mouth before taking Suboxone to help the films dissolve quickly.
Also, while it dissolves in the mouth, people should avoid:
- Cutting, chewing, or swallowing the tablet.
- Eating or drinking until the film dissolves completely.
If you’re detoxing from Suboxone, get resources about treatment counseling that works. Discover professional help from We Level Up Texas’ addiction and mental health therapists. Start getting support with a free call to our addiction hotline.
Get Help. Get Better. Get Your Life Back.
Searching for Accredited Drug and Alcohol Rehab Centers Near You? We Level Up Texas Is Opening Soon!
Even if you have failed previously and relapsed, or are in the middle of a difficult crisis, we stand ready to support you. Our trusted behavioral health specialists will not give up on you. When you feel ready or just want someone to speak to about therapy alternatives to change your life call us. Even if we cannot assist you, we will lead you to wherever you can get support. There is no obligation. Call our network hotline today.
FREE Addiction Hotline – Call 24/7Suboxone Rehab Treatment and Detox
The withdrawal symptoms linked with ceasing Suboxone use can be managed with the use of a medical detox program. Medical detox treatments typically consist of five to seven days and include 24-hour medical supervision in a supervised setting. In an inpatient environment, ongoing therapy and relapse prevention programs following detoxification might take up to 30 days.
To achieve complete healing, Suboxone use will gradually be tapered down. This process should be carried out slowly and methodically to account for the patient’s experience and stability. It is critical to form a new course for rehabilitation that could not involve taking any form of opioid medicine when Suboxone turns into an addiction, as well as if the patient no longer benefits from using the medication.
Suboxone Withdrawal Symptoms
Suboxone is often taken for prolonged periods following the cessation of other habit-forming opioids, and it may be a beneficial therapy for opiate dependency. However, if Suboxone is stopped “cold turkey,” its partial opioid agonist withdrawal symptoms are similar to those of other opioids.
Suboxone withdrawal symptoms can persist for up to a month and may include:
- Anxiety.
- Insomnia.
- Sweating.
- Nausea.
- Vomiting.
- Diarrhea.
- Abdominal pain.
- Muscle aches.
- Runny nose.
- Dilated pupils.
- Goosebumps.
- Fatigue.
- Irritability.
- Depression.
- Drug cravings.
Suboxone Withdrawal Timeline Chart
The length and quantity of Suboxone use might affect the withdrawal symptoms. Usually, after a month, the physical symptoms go away, but psychological withdrawal could persist. The first 72 hours of physical symptoms are the worst. While general discomfort is the dominant symptom in the first week, depression begins to show during the second week. A substantial probability of relapse is present if depressive symptoms and intense cravings persist after a month.
| Day/Week | Physical Symptoms | Psychological Symptoms | Risk/Notes |
|---|---|---|---|
| 1-3 | Intense physical symptoms (nausea and vomiting) | Heightened anxiety, insomnia | High risk of relapse |
| 4-7 | Transition to general discomfort | Insomnia persists, mood swings | Continued support is crucial |
| 8-14 | Depression becomes prominent | Ongoing support and aftercare are crucial | Monitor closely |
| Week 3-4 | Intense cravings, persistent depression | High risk of relapse | Critical phase |
| Beyond Week 4 | Gradual improvement in symptoms | Psychological dependence may persist | Ongoing support and aftercare are crucial |
How To Detox From Suboxone?
Detoxing from Suboxone under medical guidance can be summarized in the following:
- Medical supervision.
- Gradual tapering of dosage.
- Monitoring and management of withdrawal symptoms.
- Supportive therapies and counseling.
Medical Supervision
The partial opioid agonist buprenorphine, which is a component of Suboxone, functions on the same brain receptors as other opioids but has a weaker impact. To adjust the dosage, reduce any unfavorable effects, and assist patients in developing a stable and regulated response to Suboxone, monitoring is crucial.
Gradual Tapering of Suboxone Dosage
Tapering the amount of Suboxone gradually lowers the prescribed quantity while following physician guidance. With this method, withdrawal symptoms are lessened, and people can adjust slowly, facilitating a more seamless transition to the eventual termination of the medication-assisted treatment program.
Recommended initial tapering schedules vary, from a gradual 10% reduction weekly or monthly to a more accelerated 25% to 50% decrease every few days.
Monitoring and Management of Withdrawal Symptoms
Suboxone withdrawal monitoring and management involve evaluating psychological and physical symptoms and adjusting medication as necessary. Experts in detox treatment guarantee a well-rounded and encouraging approach that facilitates recovery.
Supportive Therapies and Counseling
Taking a step towards a drug-free life involves a holistic and evidence-based approach. Here are the most beneficial therapies you can get in an inpatient Suboxone detox:
- Cognitive-behavioral therapy.
- Mindfulness practices.
- Individual counseling.
- Group therapy.
- Art therapy.
- Holistic wellness.
- Life skills training.
- Peer support.
- Stress management.
- Relapse prevention techniques.
If you’re seeking assistance with your rehab journey, reach out to a We Level Up Texas treatment professional today—your call is free and confidential.
Opening Soon! First-Class Facilities & Amenities
World-Class High-Quality Addiction & Mental Health Rehabilitation Treatment
Coming Soon! Rehab Centers TourRenowned Addiction Centers. Serene Private Facilities. Inpatient Rehab Programs Vary.
FREE Addiction Hotline – Call 24/7Proven recovery success experience, backed by a Team with History of:
- 15+ Years Experience
- 100s of 5-Star Reviews
- 10K+ Recovery Successes
- Low Patient to Therapist Ratio
- Onsite Medical Detox Center
- Comprehensive Dual-Diagnosis Treatment
- Complimentary Family & Alumni Programs
- Coaching, Recovery & Personal Development Events
Can You Overdose on Suboxone?
While there is a very small chance of overdosing on Suboxone, people should not exceed the dose that a doctor prescribes.
Suboxone Overdose Symptoms
- Slow or shallow breathing.
- Extreme drowsiness or inability to wake up.
- Confusion or slurred speech.
- Pinpoint pupils.
- Weakness or limpness.
- Bluish tint to lips or nails.
- Nausea or vomiting.
- Loss of consciousness or unresponsiveness.
- Difficulty in coordination or motor skills.
- Respiratory distress or difficulty breathing.
In cases of Suboxone overdose:
- Seek emergency medical attention immediately.
- Call emergency services (911) or your local emergency number.
- Stay with the person experiencing the overdose and monitor their breathing.
- Do not leave the person alone.
- If trained, administer naloxone if available and follow the instructions provided.
- Provide necessary information to medical professionals, including the quantity of Suboxone taken and any other substances involved.
- Stay calm and wait for professional help to arrive.
- Do not attempt to induce vomiting unless directed by emergency services.
- Be prepared to provide CPR if the person stops breathing.
- Cooperate fully with medical professionals and follow their guidance for further treatment.

Are you seeking Suboxone detox near me? Get a free rehab insurance check without any obligation. The free rehab insurance check can help you explore several treatment options.
Inpatient Suboxone Addiction Treatment
Inpatient therapy helps to create a more regulated and encouraging atmosphere; it is highly advised for Suboxone addiction. Relapse during the early phases of rehabilitation is less likely in the controlled setting because it limits external stimuli and distractions.
Further guaranteeing a secure and efficient detoxification procedure and handling any difficulties or withdrawal symptoms is the availability of medical monitoring around the clock.
Suboxone can be tapered slowly and under medical supervision in an organized inpatient environment, which makes the withdrawal process more accessible to handle and more gradual. To provide people with a greater degree of care and support while they navigate the difficulties of eliminating Suboxone dependency and building a foundation for sustained recovery, this all-encompassing approach takes into account both the medical and psychological elements of Suboxone addiction.
We Level Up Texas Suboxone Detox
Detoxing from Suboxone calls for special care, and We Level Up Texas is your reliable guide on this road to recovery.
Providing individualized care and guaranteeing a safe and efficient detox procedure that is tailored to meet your specific requirements is the mission of our caring and professional staff.
Our goal at We Level Up Texas Suboxone rehab center is to support you. At the same time, together, we can navigate the difficulties of Suboxone detox and pave the way for long-term recovery by emphasizing personalized, evidence-based treatment. Contact us today to begin your journey to a drug-free life with confidence and support.
Opening Soon! World-class, Accredited, Anticipated 5-Star Reviewed, Effective Addiction & Mental Health Programs. Complete Behavioral Health Inpatient Rehab, Detox plus Co-occuring Disorders Therapy.
FREE Addiction Hotline – Call 24/7End the Addiction Pain. End the Emotional Rollercoaster. Get Your Life Back. Start Drug, Alcohol & Dual Diagnosis Mental Health Treatment Now. Get Free No-obligation Guidance by Substance Abuse Specialists Who Understand Addiction & Mental Health Recovery & Know How to Help.
How Long Do Opiates Stay in Your System (Urine, Blood, Hair, and Saliva) | Informative Video
Start a New Life
Begin with a free call to an addiction & behavioral health treatment advisor. Learn more about our dual-diagnosis programs. The We Level Up treatment center network delivers recovery programs that vary by each treatment facility. Call to learn more.
- Personalized Care
- Caring Accountable Staff
- World-class Amenities
- Licensed & Accredited
- Renowned w/ 100s 5-Star Reviews
We’ll Call You
Search We Level Up Texas Suboxone Addiction, Detox Topics, and Resources
Sources
- Kumar R, Viswanath O, Saadabadi A. Buprenorphine. [Updated 2023 Nov 30]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK459126/
- Blum K, Oscar-Berman M, Femino J, Waite RL, Benya L, Giordano J, Borsten J, Downs WB, Braverman ER, Loehmann R, Dushaj K, Han D, Simpatico T, Hauser M, Barh D, McLaughlin T. Withdrawal from Buprenorphine/Naloxone and Maintenance with a Natural Dopaminergic Agonist: A Cautionary Note. J Addict Res Ther. 2013 Apr 23;4(2):10.4172/2155-6105.1000146. Doi: 10.4172/2155-6105.1000146. PMID: 24273683; PMCID: PMC3835595.
- Srivastava AB, Mariani JJ, Levin FR. New directions in the treatment of opioid withdrawal. Lancet. 2020 Jun 20;395(10241):1938-1948. Doi: 10.1016/S0140-6736(20)30852-7. PMID: 32563380; PMCID: PMC7385662. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7385662/
- How does Suboxone work for addiction? Velander JR. Suboxone: Rationale, Science, Misconceptions. Ochsner J. 2018 Spring;18(1):23-29. PMID: 29559865; PMCID: PMC5855417. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5855417/ Related review for Can you get addicted to Suboxone? Is Suboxone addictive drug? Can you become addicted to Suboxone? Does Suboxone help with addiction?
- Sivils A, Lyell P, Wang JQ, Chu XP. Suboxone: History, controversy, and open questions. Front Psychiatry. 2022 Oct 28;13:1046648. Doi: 10.3389/fpsyt.2022.1046648. PMID: 36386988; PMCID: PMC9664560. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9664560/
- Shulman M, Wai JM, Nunes EV. Buprenorphine Treatment for Opioid Use Disorder: An Overview. CNS Drugs. 2019 Jun;33(6):567-580. Doi: 10.1007/s40263-019-00637-z. PMID: 31062259; PMCID: PMC6585403. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6585403/
- Jahan AR, Burgess DM. Substance Use Disorder. [Updated 2023 Jul 21]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK570642/
- Blanco C, Wiley TRA, Lloyd JJ, Lopez MF, Volkow ND. America’s opioid crisis: the need for an integrated public health approach. Transl Psychiatry. 2020 May 28;10(1):167. Doi: 10.1038/s41398-020-0847-1. PMID: 32522999; PMCID: PMC7286889. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7286889/
- Dydyk AM, Jain NK, Gupta M. Opioid Use Disorder. [Updated 2023 Jul 21]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK553166/ Related study to Outreach Suboxone and MAT Addiction Clinics; Suboxone uses other than addiction; Suboxone for meth addiction.
- Berge KH, Seppala MD, Lanier WL. The anesthesiology community’s approach to opioid- and anesthetic-abusing personnel: time to change course. Anesthesiology. 2008 Nov;109(5):762-4. Doi: 10.1097/ALN.0b013e31818a3814. PMID: 18946282. https://pubmed.ncbi.nlm.nih.gov/18946282/